Trust in Medicine, the Health System & Public Health
This essay reviews more than forty years of public opinion polling to look at trust in medicine, the health system, and public health. We use polling data to explore the reasons for the decline and current level of public trust in leaders of medicine and public health, including underlying forces such as the decline in trust in other institutions. Except for the military, none of the efforts to improve public trust in various institutions have been very successful to date. Given the uncertainty about how to restore trust, this essay makes a number of recommendations that might improve public trust in medicine and public health in the future.
A discussion of trust in medicine, the health system, and public health needs to recognize as context the exceptionally low trust the American public currently has in institutions, especially government.
As many scholars have noted, trust in the federal government has declined sharply over the past decades.1 In 1958, nearly three-fourths (73 percent) of the public believed they could trust the federal government to do what is right just about always or most of the time. By 1980, trust had dropped to 25 percent, and although the level of trust has varied, at no time since 2006 has more than one-third of the public expressed trust in the federal government. Currently only one in five U.S. adults (20 percent) believe they can trust the government in Washington to do what is right just about always or most of the time.2
When President Johnson signed the Medicare and Medicaid Act of 1965, more than three-fourths (77 percent) of the U.S. public said they trusted the government to do what is right just about always or most of the time.3 No doubt trust in the federal government contributes both to support of and opposition to government-led changes in the health care system.
The level of public trust in national governments worldwide appears to have affected public trust in public health recommendations during the COVID-19 pandemic. A recent study of data from 177 countries found that higher levels of trust in the national government have a large association with lower COVID-19 infection rates and, among middle-income and higher-income countries where vaccine availability was more widespread, also correlate with higher COVID-19 vaccination rates.4
Confidence in a variety of other institutions in the United States has also declined during the past fifty years. For instance, Gallup has found that the share of the public expressing a great deal of confidence in public schools has fallen from 58 percent in 1973 to 32 percent in 2021; in banks, from 60 percent in 1979 to 33 percent in 2021; and in television news, from 46 percent in 1993 to 16 percent in 2021. Even confidence in organized religion has declined, from 65 percent having a great deal of confidence in 1973 to 37 percent in 2021.5
Given the overall downward trend in trust in institutions, it is not surprising that trust in medicine has also decreased. Although comparable data on trust in the medical system going back to the 1960s are not available, data on trust in the leaders of medicine have been collected since then. The Harris Poll shows that the share of the public expressing a great deal of confidence in “the people in charge of running” medicine had already fallen from 73 percent in 1966 to 57 percent in 1973, and eventually to 34 percent in 2012.6NORC’s General Social Survey also finds that the public’s trust in the leaders of medicine declined significantly since the 1970s. In 1974, a majority of the public (54 percent) expressed a great deal of confidence in “the people running” medicine. Confidence peaked at 61 percent in 1976. In contrast, fewer than four in ten adults (38 percent) in 2021 said they had a great deal of confidence. Throughout most of this forty-seven-year period, partisan differences were modest, except in the late 1980s and early 1990s, when a larger share of Republicans than Democrats expressed confidence. But in 2021, Democrats were more likely than Republicans (46 percent to 32 percent) to say they had a great deal or quite a lot of confidence in the people running medicine, and the change was mainly among Democrats (Figure 1).7
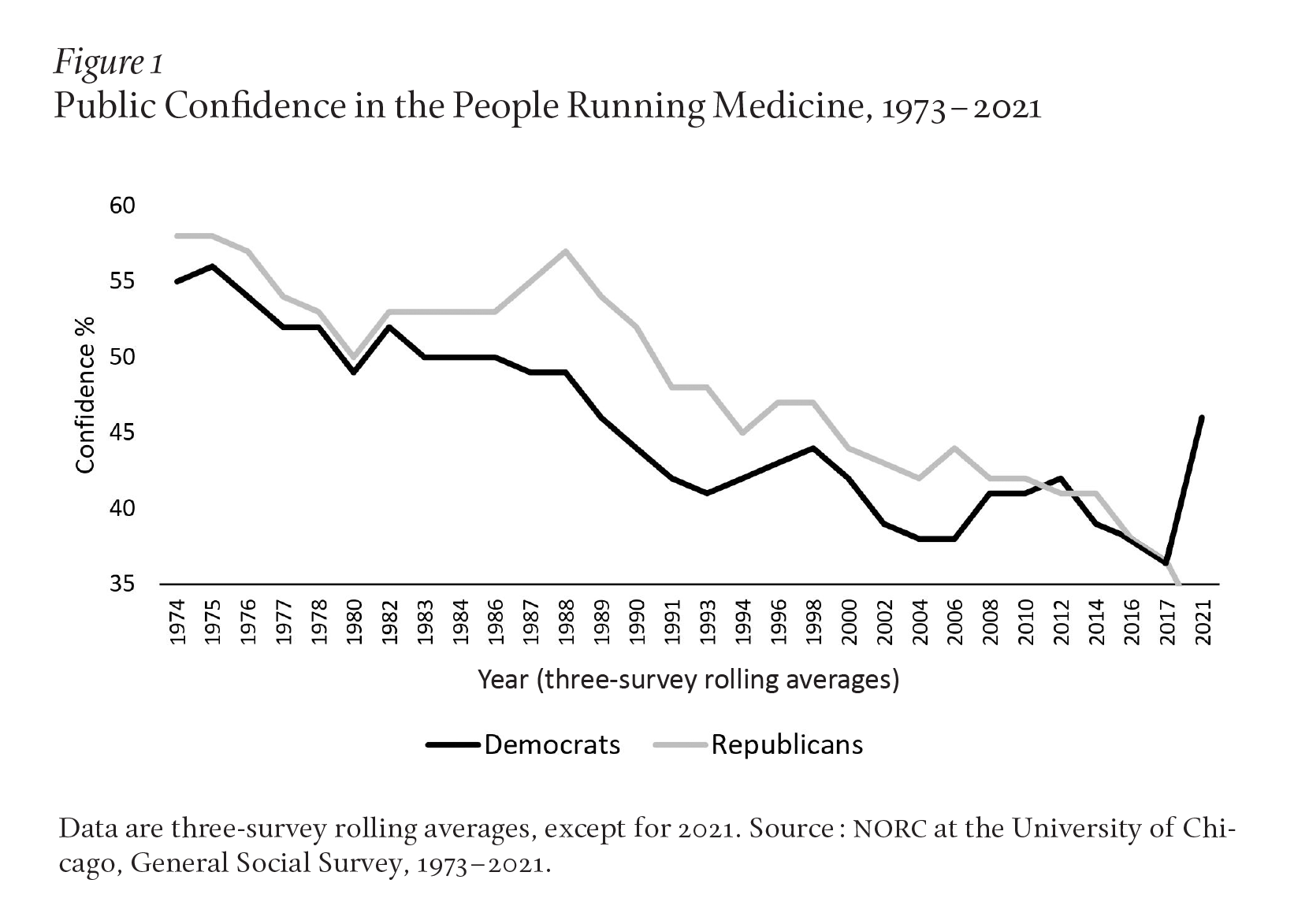
The partisan difference in 2021 is likely related to the government’s response to COVID-19. Leaders of medicine supported recommendations made by public health officials for responding to the pandemic that included lockdowns, mandatory vaccination, and mask requirements. Democrats were more likely to favor these steps than Republicans, a large share of whom opposed such measures.8 It is too early to tell whether the pattern of partisan difference on confidence in the leaders of medicine will persist.
Views of the medical system do not appear to be dramatically different from views of its leaders. From 1993 to 2019, Gallup asked about the nation’s medical system and, during that period, only 34 percent to 44 percent of the U.S. public expressed a great deal or quite a lot of confidence in it. Public confidence in the nation’s medical system increased during the first year of the COVID-19 pandemic, from 36 percent in 2019 to 51 percent in 2020, before declining to 44 percent in the summer of 2021.9 By then there were significant partisan differences, with 50 percent of Democrats (including those who lean Democratic) and 36 percent of Republicans (including leaners) expressing confidence.10
When we look at the issue of public trust in medicine, it is important to separate trust in the medical profession from people’s trust in their own personal doctors. The results of a twenty-nine-country survey found something unique about the United States: it ranked near the bottom (tied for twenty-fourth) in the public’s trust in the medical profession but near the top (third) in patients’ satisfaction with their own medical care when they last visited a doctor. It appears that compared with the United States, the public elsewhere sees the leaders of medicine in their countries as being closer to their own views in the actions they take.11
The evidence clearly shows that the U.S. public’s trust in medicine is not related to individuals’ perception of the quality of care they receive. A recent poll found that more than eight in ten U.S. adults (82 percent) rated the quality of health care they receive as excellent or good, 16 percent as only fair or poor.12 When it comes specifically to their own doctor, 76 percent of those who have a regular doctor rate the medical care they have received in the past twelve months from their regular doctor’s office or clinic as excellent or very good, 16 percent as good, and 7 percent as fair or poor.13 What this result suggests is that, at least among those who have a regular doctor and are able to receive medical care, there are other factors that drive public distrust of the leaders of medicine.
When asked in general terms how much they trust various private groups involved in health and health care, none of the groups are completely trusted by a majority of the public, but some are more trusted than not. When it comes to trusting the groups completely or somewhat, health care practitioners—nurses and doctors—come first, with 85 percent trusting nurses completely (32 percent) or somewhat (53 percent) and 84 percent trusting doctors completely (28 percent) or somewhat (56 percent). Trust drops for hospitals (14 percent trust completely, 58 percent somewhat), but still more people trust them than not. The tables are turned for pharmaceutical companies and health insurance companies. Only about one-third of the public trusts pharmaceutical companies (3 percent trust completely, 31 percent somewhat) or health insurance companies (4 percent trust completely, 29 percent somewhat).14
Among fifteen groups that were rated on their honesty and ethical standards, nurses (89 percent), doctors (77 percent), and pharmacists (71 percent) along with grade-school teachers (75 percent) are the top four groups in terms of being rated highly or very highly. By contrast, members of Congress rate at the bottom of the list, tied with car salespeople (8 percent each).15
Turning to the public health system, in the middle of the COVID-19 pandemic, during which more than one million have died so far in the United States, only about one-third of adults (34 percent) gave positive (excellent or good) ratings to the nation’s system for protecting the public from health threats and preventing illness, with nearly two-thirds (65 percent) rating the nation’s public health system as fair or poor. Democrats (40 percent) were more likely than Republicans (30 percent) to rate the public health system positively, Latinos (45 percent) more likely than Whites (33 percent), and adults from households with incomes under $35,000 per year (43 percent) more than those with incomes $35,000 or over (30 percent). But no major demographic group gives the public health system a majority-positive rating. Of note, even in the absence of a pandemic in 2009, only 43 percent gave positive ratings to the nation’s public health system (Figure 2).16
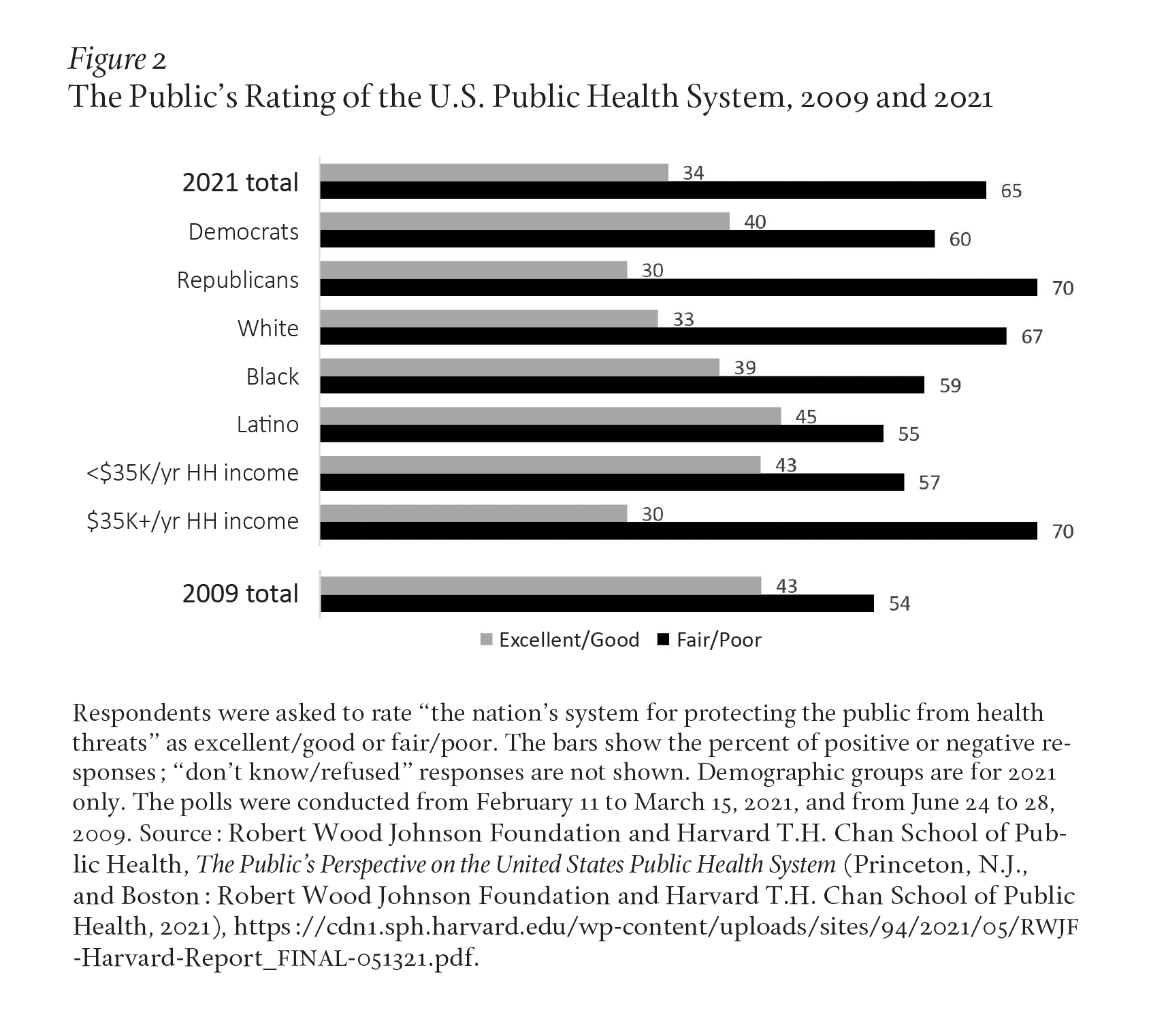
Polls show that the public does not express a high level of trust in government public health agencies or leaders when it comes to the broad question of making recommendations to improve health. Less than half of the public says they trust (a great deal or quite a lot) the recommendation of their state health department (41 percent), the surgeon general (40 percent), and the federal Department of Health and Human Services (33 percent). Once again, the public rates nurses (71 percent), health care workers they know (70 percent), and doctors (67 percent) at the top of the list.17
The Centers for Disease Control and Prevention (CDC) and the Food and Drug Administration (FDA) are sister agencies that work to protect the public health but have different responsibilities. The CDC’s mission is to collaborate to create the expertise, information, and tools that people and communities need to protect health through health promotion; prevention of disease, injury, and disability; and preparedness for new health threats. The FDA is a regulatory agency whose mission is to protect the public health through the regulation of food, cosmetics, tobacco, and medical products, including drugs, biological products, and medical devices. This includes the principal responsibility for making fundamental decisions about approving new drugs and vaccines for use and monitoring for adverse effects resulting from them.18
An October 2021 poll found that the public did not trust medical advice from either the CDC or the FDA at a high level (“a lot”), but a significant share trusted medical advice from them at least somewhat. About half of the public (51 percent) said they trusted medical advice from the CDC a lot (29 percent) or somewhat (22 percent). Similarly, half of the public (50 percent) trusted medical advice from the FDA a lot (21 percent) or somewhat (29 percent). Although the CDC and FDA play very different roles, the ratings of the two agencies were about the same. But once again, there were significant partisan differences. More than eight in ten Democrats trusted medical advice from the CDC (85 percent) and FDA (80 percent) a lot or somewhat, compared with only about three in ten Republicans (30 percent CDC, 31 percent FDA).19 When it came specifically to confidence in sources of information about coronavirus vaccines, less than half of the public in September 2021 expressed a great deal or quite a lot of confidence in the CDC (45 percent) and FDA (38 percent) as sources.20 In January 2022, 44 percent of the public said they trusted what the CDC has said about the coronavirus, a marked decline since the early months of the COVID-19 pandemic, when in April 2020 more than two-thirds (69 percent) reported that they trusted what the CDC said about the virus.21
In a country in which about half of the public does not express trust in public health agencies, how does that distrust influence real-world health decisions? When those who said they would not or might not get a coronavirus vaccine were asked about their reasons, three of the top four reasons reflected a distrust in government or other institutions: the vaccine was too untested and they would wait to see what happens (58 percent), they do not trust government (37 percent), or they do not trust the scientists and companies that make the vaccine (28 percent). Only one of the top four reasons referenced individual medical conditions, as 37 percent of the people expressed worry about allergies or side effects.22
What are the reasons for public distrust in the leaders of medicine? Prior research suggests that the public judges the performance of an institution based on how it addresses the key issues that are most important to them. If leaders do not address the big issues, it will have a negative effect on public confidence.23 Polls have shown over the past several years that when it comes to health care, apart from COVID-19, the most important issue to the public is the high cost of health care and prescription drugs for individuals.
When the public was asked in January 2020, shortly before the beginning of the COVID-19 pandemic, how important each of twenty-two possible domestic priorities should be for President Trump and Congress during the rest of the year, the top two priorities were taking steps to lower the cost of health care (80 percent extremely or very important) and to lower prescription drug prices (75 percent). And there was both Democratic (89 percent and 85 percent, respectively) and Republican (76 percent and 69 percent, respectively) support for these priorities, with partisans of both parties ranking them higher than another shared priority, reducing the federal budget deficit (60 percent for Democrats and 65 percent for Republicans).24 Increasing federal funding for K–12 public education and reducing hate crimes both received 63 percent support, but partisans differed dramatically in their support for them.
In December 2020, during the COVID-19 pandemic, the public was asked which of twenty-three possible priorities for President-elect Biden and the new Congress they felt were extremely important. Overall, the public wanted to address the destructive effects of COVID-19: four of the top five priorities were related to coping with the impact of COVID-19 on people’s lives and on the economy. But the second highest priority in the public’s mind was the federal government taking action to lower prescription drug prices.25
In September 2021, at the time of congressional debate over the $1 trillion infrastructure bill and the then-$3.5 trillion social spending bill, the public was asked the importance of including each of twenty proposed items in these spending bills. The top priority was for the federal government to negotiate directly with pharmaceutical companies to lower the prices of prescription drugs for seniors on Medicare.26
Polls have shown that the public sees doctors and hospitals as major contributors to high health care costs, the public’s biggest health care concern. In 2019, nearly three-fourths of the public believed that high prices charged by hospitals were a “major cause” of high health care costs, and about two-thirds thought that high prices charged by doctors and other health professionals were a “major cause.”27 Clearly, these groups are not seen as leaders in trying to resolve what the public sees as the biggest health care issue.
In addition, for Black Americans, racism in American life is a fundamental problem. Nearly three of every four Black Americans say that civil rights is a “very important” issue.28 This concern includes discrimination in health care.29 More than three-fourths of the public as a whole say it is very important that all Americans are treated equally in terms of the health care they receive (77 percent). Nearly nine in ten (88 percent) U.S. adults say it is very important that African Americans receive the same quality of health care as White Americans.30
What are the underlying reasons for public distrust of the public health system? There are several, but we will focus on two: overall distrust of the federal government and the absence of a high level of trust in medical scientists and in scientists more generally.
Although the public has considerable confidence in science as an institution, it has less confidence in individuals involved in scientific endeavors. Nearly two-thirds (64 percent) express a great deal or quite a lot of confidence in science as an institution.31 However, only about four in ten U.S. adults (39 percent) say they have a great deal of confidence in scientists to act in the best interests of the public, while 48 percent have a fair amount of confidence and 12 percent say they have not too much or no confidence at all. Similarly, only 43 percent report that they have a great deal of confidence in medical scientists to act in the best interests of the public, while 46 percent have a fair amount of confidence and 11 percent say they have not too much or no confidence at all. Distrust is especially acute among Black respondents, of whom only 27 percent have a great deal of confidence in scientists and 35 percent in medical scientists. Indeed, only 53 percent of college graduates could muster a great deal of confidence in medical scientists and 50 percent in scientists. And here as in so many areas, the partisan divide is greater than 20 percentage points.32
Democrats are significantly more likely than Republicans to express a great deal of confidence in scientists in general (52 percent to 27 percent) and in medical scientists (53 percent to 31 percent) to act in the public’s best interest. In addition, Black Americans are significantly less likely than both Whites and Latinos to have a great deal of confidence in scientists in general (Blacks 27 percent, Whites 41 percent, Latinos 39 percent) and in medical scientists (Blacks 35 percent, Whites 43 percent, Latinos 45 percent). College graduates are more likely than non–college graduates to express a great deal of confidence in both scientists in general (50 percent of college graduates, 34 percent of non–college graduates) and in medical scientists (53 percent versus 38 percent).33
A critical difference is that a majority of Republicans think many scientists have agendas beyond the pursuit of scientific facts. While 54 percent of U.S. adults believe that scientists make judgments solely based on the facts, 45 percent believe scientists’ judgments are just as likely to be biased as other people’s. Seventy-three percent of Democrats believe that scientists make judgments solely on the facts, while more than two-thirds of Republicans (68 percent) think that scientists’ judgments are just as likely as other people’s to be biased.34
Public confidence in colleges and universities, the home of many scientists, displays a similar partisan split. While more than half of Democrats (56 percent) say they have a great deal or quite a lot of confidence in colleges and universities, this view is shared by only one-third of Republicans.35 This partisan split is part of a change that has taken place over the past several years. In 2017, two-thirds (67 percent) of Democrats (including those who lean Democratic) and more than half (53 percent) of Republicans (including leaners) believed that colleges and universities had a positive effect on the way things are going in the country. In 2019, the attitudes of Democrats/leaners had not changed (still 67 percent), while positive assessments among Republicans/leaners declined to 33 percent.36 By 2021, about three-fourths of Democrats (76 percent) but only one-third of Republicans (34 percent) said that colleges and universities had a positive effect.37
Public distrust of government and medical experts was reflected in the early-2010s debate over the creation of a comparative effectiveness agency for health care in the United States. Despite the fact that such agencies exist in Canada and Great Britain, a majority (56 percent) of U.S. adults opposed having a government decision-making body that recommends whether government programs should pay for prescription drugs or medical/surgical procedures if they think they cost too much. One in two Democrats supported such a decision-making body, as compared with only about one in four Republicans (27 percent).38
The forces of distrust in the health field are exacerbated by the deep political polarization that has developed in the United States, particularly over the past two decades. Since the mid-1990s, those identifying with the two political parties have grown further apart in their overall policy preferences. In 2019, average Republicans differed from average Democrats by 39 percentage points in their views across thirty policy-related priorities, more than double the gap in 1994.39 The differences between the parties encompass not only critical health policy and social issues—particularly abortion—but also issues relating to the preferred role for government in addressing critical national problems and even some of the responses to the COVID-19 pandemic. According to political scientists Nolan McCarty, Keith Poole, and Howard Rosenthal, partisan polarization is now at its highest point in at least a century.40
A substantial body of research shows that votes on policy issues by individual members of Congress often do not correspond to overall public opinion. In recent years, votes by members more closely reflect the views of their party’s identifiers than the voting public. Because those who identify with a party are most likely to have voted in a partisan primary election and are often more active in political affairs, their views have more influence on the voting behavior on members of Congress of the same party.41 As a result, differences in attitudes between Democrats and Republicans in the general public and among voters are especially important politically. As adherents of the two parties have become more polarized in their views, so have votes in Congress. An important consequence is that legislation on health care, as on many other policy areas, differs significantly depending on which party is in power.
Political polarization is evident on several values and policies related to health care and public health. Overall, when it comes to the federal government’s role in health care, about half of the public prefers that the federal government be less involved (30 percent) or about as involved as it is now (21 percent), while 46 percent believe it should be more involved. But more important is the sharp partisan split: only 17 percent of Republicans want the federal government to be more involved in health care, while 68 percent of Democrats do.42 In addition, most Democrats (86 percent) favor substantially increasing federal spending on improving the nation’s public health programs. This view is shared by only four in ten Republicans.43 We have already seen that Democrats have a significantly higher level of confidence than Republicans in medical scientists and scientists in general to act in the best interest of the public, and are more likely to believe scientists make judgments based solely on facts.44
Although 82 percent of Democratic likely voters in the 2020 election believed that making sure all Americans have health care coverage is the responsibility of the federal government, that view was shared by only 39 percent of Republican voters.45 More than nine in ten Democrats (93 percent) favor keeping the existing Affordable Care Act and passing additional legislation to improve how it works. Only three in ten Republicans (30 percent) have this view.46
Over the forty-year period of falling public trust in institutions, efforts to restore public trust have accomplished little. Political scientists Jack Citrin and Laura Stoker have lamented, in the more general context of trust in government, “recommendations about how to raise the level of political trust tend to have a forlorn quality.” They add that partisan polarization is “a formidable barrier to the rapid restoration of trust.”47 Some scholars have suggested that with changes in the nation’s culture, the decline in trust might eventually reverse, but we have not seen any supporting evidence to date.48
The exception is the U.S. military. Since the mid-1970s, the military has been the only major institution to increase its confidence ratings.49 What lessons can we learn from the increase in public trust in the military? The first, applicable directly to the military, is to avoid involvement in unpopular wars. But there are more. When those who expressed confidence in the military were asked by Gallup in an open-ended question why they had such confidence, four issues emerged: competence, the importance of the job they do, personal connections (for example, the respondent, a friend, or a family member served in the military), and positive attitudes about people who serve. In addition, 68 percent of the public felt that the phrase “personally courageous” described military leadership “very well.”50 While these responses offer some hope for improvement in public trust in other institutions, the perceived importance of the military’s role and personal courage of military leaders make the example harder to emulate. It is too early to know if the gravity of COVID-19 will inspire similar public trust in leaders of medicine and public health.
How might the public’s trust in medicine be recovered? It is not what individual physicians are doing with patients that is driving distrust in the leaders of medicine. Prior research suggests that the public judges the performance of institutions based on how they address the key issues that are most important to them. Leaders of medicine need to be seen as addressing what the public believes are the biggest health care problems in the United States.
In particular, leaders of medicine and hospitals would have to take firm positions on the best way to solve the problems of high health care and drug costs. As noted earlier, the public sees doctors and hospitals as the leading causes of the problem of high health care costs. In this regard, it is important that physician and hospital organizations’ public positions do not look like they are economically self-serving. In addition, they need to focus on racial/ethnic equity. In taking policy positions, it is important that their stands be publicly visible, particularly in the media.
How might the public’s trust in public health be recovered? In this environment of political polarization, restoring trust is a difficult goal. But there are six initiatives that deserve our focus.
First, key federal and state public health officials should be more visible to the public, with a focus on their backgrounds and commitment. Much of the public is unsure of what public health leaders and professionals do to help them and their families directly. Despite extraordinary efforts and sacrifices by public health officials during the COVID-19 pandemic, positive public perception of leaders of public health has not reached or increased at the rate of the military over recent decades. And unlike doctors and nurses, whose heroic acts during the pandemic have been covered widely by the media, almost no attention has been paid to the heroic deeds of public health officials who work for health departments administering vaccinations, COVID-19 tests, and contact tracing in often dangerous settings, or to leaders who face threats of violence simply for trying to serve the public.
Second, it is important that public health leaders not be seen as associated with one or the other political party. Public health agencies and advisory groups should be separated as much as possible from political decision-makers when making their public health recommendations.
Third, because of the political polarization by religion, race/ethnicity, and region, it is important to have scientific spokespeople who are clearly identified with each demographic group across the country.
Fourth, because a substantial share of the public does not have confidence in scientists’ advice, it is necessary for public health leaders to explain more fully the nature of the scientific findings that lead to their policy recommendations. It is not enough to say, “Scientists believe this, so here is what you should do.”
Fifth, state and local health departments should make efforts to offer information on health across the entire population, so a larger share of the public has experience with them before a health emergency occurs. Prior to COVID-19, surveys showed that few people had contact with state and local health agencies. Only 22 percent of the public said they had any contact with a local or county government health agency in the past twelve months. Even fewer (14 percent) had contact with a state government health agency.51 The public has strong interest in consumer health information and advice about issues affecting the health of their families. Public health agencies should be seen as credible sources for such vital recommendations.52
Sixth, when the COVID-19 pandemic finally comes to an end (or settles on some steady state), it is important to have a bipartisan examination of what can be done to reduce the high level of politicization of the response to pandemics that may occur in the future.
If we cannot reduce the levels of distrust of leaders of medicine and public health, we are likely to see continuing conflicts between those leadership groups, the political parties, and the public on critical public health and medical science issues
